Published - Sat, 30 Jul 2022
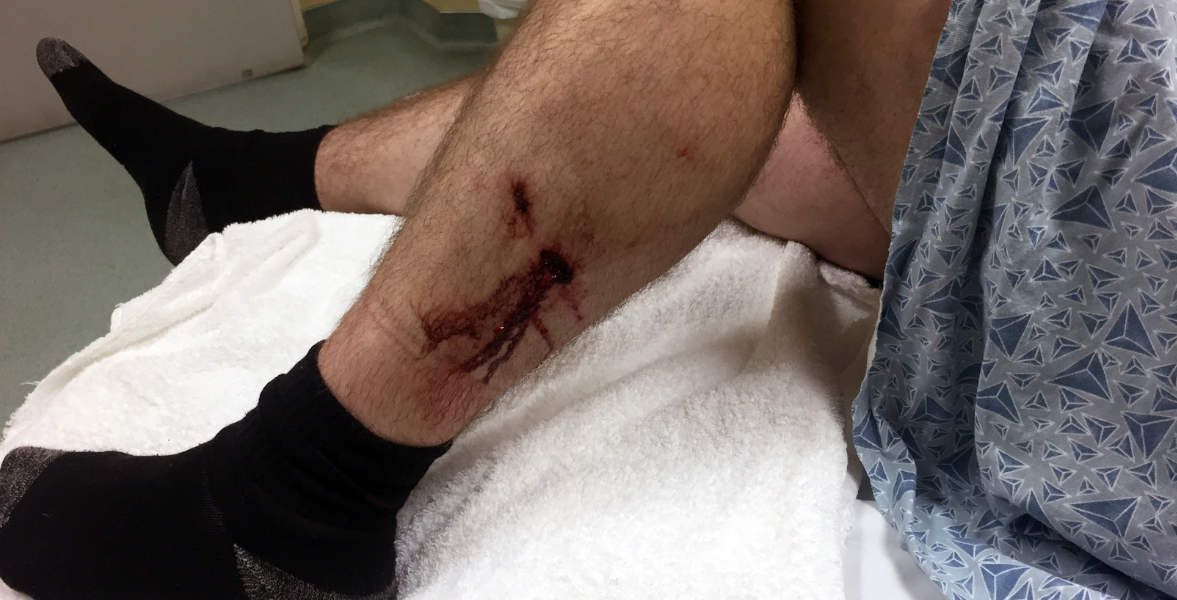
Dos and Don’ts during Dog Bite
Dog bites account for up to 90% of all animal bites. 4.5 million dog bites occur every year within the U.S., and quite 27,000 victims need surgical intervention. Injuries could be deep that involve structures such as skin as well as muscles, bones, nerves, and blood vessels. It could result in dangers of acquiring infections, or even tetanus after a bite.
Wound cleansing decreases the danger of infections from dog bites.
After confirming that the victim is medically stable, physicians begin a primary assessment by taking a history. Many medical conditions place a patient at high risk of wound infection from a bite
Dogs have rounded teeth, and it's the pressure exerted by their jaws may cause vital injury to the tissues beneath the skin, as well as bones, muscles, tendons, blood vessels, and nerves.
The risk of being bitten by a dog will increase if there's a dog within the home. Males are more frequently bitten by dogs than girls.
Children between the ages of five and nine are bitten by a dog more than adults and they need medical attention.
Dos during Dog Bite -
If a dog bites you or somebody with you, take the person to a secure place far from the dog to stop any further attack and injury.
Infants and kids should be evaluated for any bite.
If there aren't any signs of skin injury or if there's any abrasion from a bite, it will be great to observe for signs and symptoms of infection (pain, redness, warmth, swelling, and emptying of pus or fluid) before seeking treatment.
If the skin is unbroken, clean the bite with water.
Gather data from the dog's owner concerning the dog's immunization status if possible.
Since dog bites can cause vital injury to structures under the skin, a kind of injury that can't invariably simply be seen.
Moreover, if there's pain at or close to the bite, underlying tissues and alternative structures are affected, or if the bite disrupts the skin by inflicting a puncture, laceration, or tear, immediately visit a doctor or Emergency Department.
Prevention –
Dog bites usually occur once there's miscommunication between the dog and the victim. It’s not common to have an unmotivated attack by a stray dog. Often, it's the dog owner or a loved one who is bitten.
To stop being bitten by a dog: Choose a dog breed that's compatible with the family.
Aggressive dogs might not be suitable in the home with infants and little youngsters.
Dogs are social animals; thus, socialization and coaching can facilitate and minimize the danger of dog bites.
Do not approach a stray or strange dog.
Do not approach a dog with fast motions/speed.
Give some time for the dog to acknowledge your presence before attempting to pet it.
Will I get rabies?
If the dog is not immunized, take an antirabies injection right after the bite along with a Tetanus shot.
If treatment is initiated promptly following a bite, rabies can be prevented. If exposure isn't treated and a person develops clinical signs, he/she may sometimes end up in death.
Created by
Comments (0)
Search
Popular categories
Latest blogs
All you need to know about Syphilis
Tue, 15 Nov 2022

What is Pemphigus Vulgaris?
Tue, 15 Nov 2022
Know about Scorpion Stings
Sat, 12 Nov 2022

Write a public review