Published - Tue, 18 Oct 2022
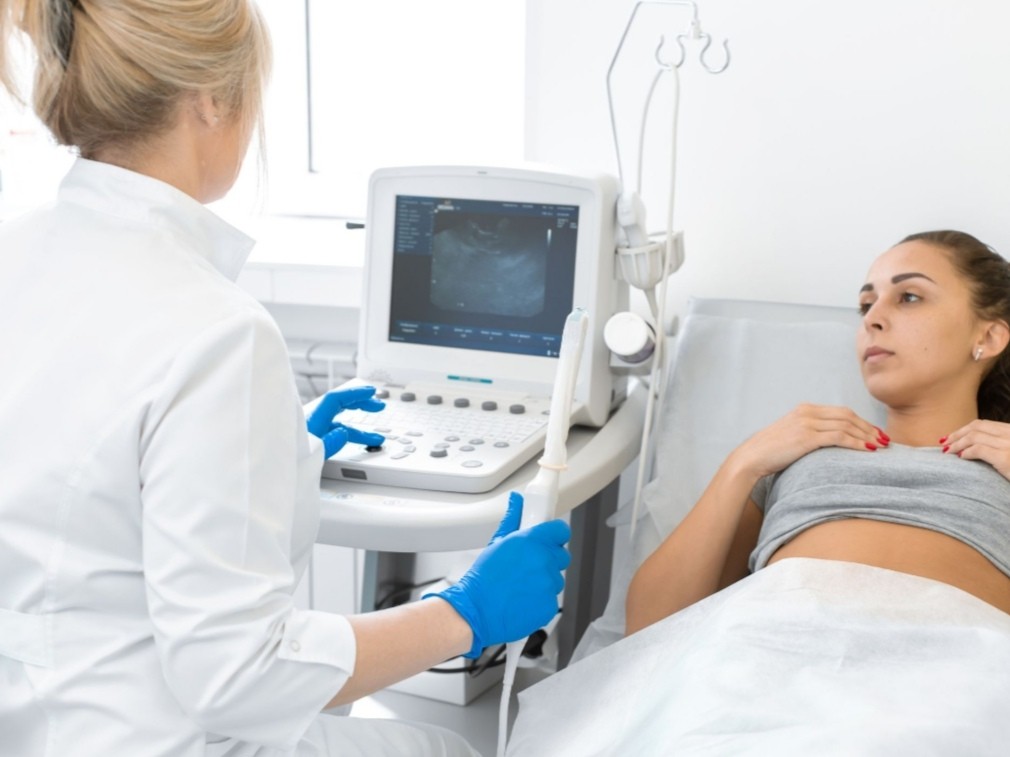
Ectopic Pregnancy: Evaluation & Treatment
EVALUATION
The incidence of detected ectopic pregnancies has increased fivefold over the last 20 years due to increasingly sensitive screening aids.
1. Stabilization: It is important to establish the airway, respiratory, and cardiovascular status immediately before making a diagnosis. Two large-bore peripheral lines are secured for fluid and blood resuscitation.
2. Laboratory studies
a) Urine pregnancy test: A urine sample can provide a quick qualitative β–human chorionic gonadotropin (β-hCG) screen and most screens with increasing sensitivity, now at approximately 4 weeks gestational age.
b) Blood work: Blood typing and screening, Rh sensitivity, quantitative β-hCG level, and a CBC are sent immediately. Β-hCG levels normally double every 36 to 48 hours. Levels in abnormal pregnancies do not increase as rapidly and may plateau or decline. Thus, if they are available, serial levels are useful in establishing a growth pattern.
3. Ultrasonography: A distinct fetal body and fetal cardiac activity can be detected ultrasonographically by 6 weeks gestation (transvaginal) or 7 weeks gestation (transabdominal), making the search easier for the ectopic site at this stage. There must be two distinct echogenic layers (i.e., the decidua vera and the decidua capsularis) surrounding the gestational sac before the diagnosis of intrauterine pregnancy can be made.
THERAPY
1. General therapy: All Rh-negative mothers are given Rho(D) immune globulin in a single intramuscular dose to prevent potential maternal Rh antibody formation. Can be within 72 hours of the initial bleeding episode
2. Specific therapy
a) Unruptured ectopic pregnancy: These patients are hemodynamically stable. Treatment options include:
— Laparoscopic salpingostomy and ectopic excision
— Nonsurgical treatment with methotrexate, leucovorin, or mifepristone
— Salpingocentesis (i.e., transvaginal needle aspiration of the gestational sac, potentially with direct injection of methotrexate)
b) Ectopic pregnancy without cardiac activity: Patients with a serial decline of β-hCG levels and no evidence of erosion or rupture on repeat sonography may be managed nonoperatively by the obstetrician. Medications may be used to induce expulsion. Laparoscopic intervention is performed if there is any sign of erosion or rupture.
c) Ruptured ectopic pregnancy: These patients may be hemodynamically unstable and therefore require aggressive fluid and blood resuscitation and control of bleeding. Laparoscopic ectopic excision via salpingectomy is indicated.
DISPOSITION
1. A hemodynamically stable patient with a history of abdominal pain, vaginal bleeding, or both; a benign examination; and ultrasound revealing no clear evidence of ectopic or intrauterine pregnancy may be discharged with strong ectopic precaution warnings. These patients should see an obstetrician in 48 hours for a repeat examination and quantitative β -hCG levels. Ultrasound is repeated in 2 to 7 days to search for pregnancy.
2. A hemodynamically stable patient with a history of abdominal pain, vaginal bleeding, or both with abdominal or adnexal tenderness on physical examination, and evidence of cul-de-sac fluid accumulation on ultrasound but no clear evidence of intrauterine pregnancy should be admitted for observation, serial abdominal examinations, repeat quantitative β-hCG levels (in 36 to 48 hours), and repeat sonography.
3. A hemodynamically stable patient with or without abdominal or adnexal tenderness and sonographic evidence of ectopic pregnancy is admitted.
4. A hemodynamically unstable patient with pregnancy by qualitative β-hCG requires aggressive resuscitation en route to the operating room.
Created by
Comments (0)
Search
Popular categories
Latest blogs
All you need to know about Syphilis
Tue, 15 Nov 2022

What is Pemphigus Vulgaris?
Tue, 15 Nov 2022
Know about Scorpion Stings
Sat, 12 Nov 2022

Write a public review